Do you google your symptoms and get the answer of hypothyroidism? You then ask your doctor to test your thyroid, and everything comes back “normal.” Frustrating right? How is it possible to have such evident thyroid dysfunction, but have it appear normal on lab work? The answer is that your body is compensating. Our bodies have a built-in stress response that is meant to protect us and keep us alive. Stress is not bad. It is when we have too much stress on a system that is already compensating that we begin to see issues.
How does stress interfere with our metabolism?
In my Stress and Metabolism series, I wrote on the compensation of the body. I will highlight some of the key points here. Our bodies try to compensate and make up for these things by releasing our stress hormone, cortisol, which leads to us being in a chronically stressed-out state. When the body is in a stressed state, it does not prioritize hormone production or digestion and puts increased demand on the thyroid. For this reason, the symptoms arise. When our bodies are in this stressed state for too long, here’s what happens:

How does stress impact our thyroid hormones?
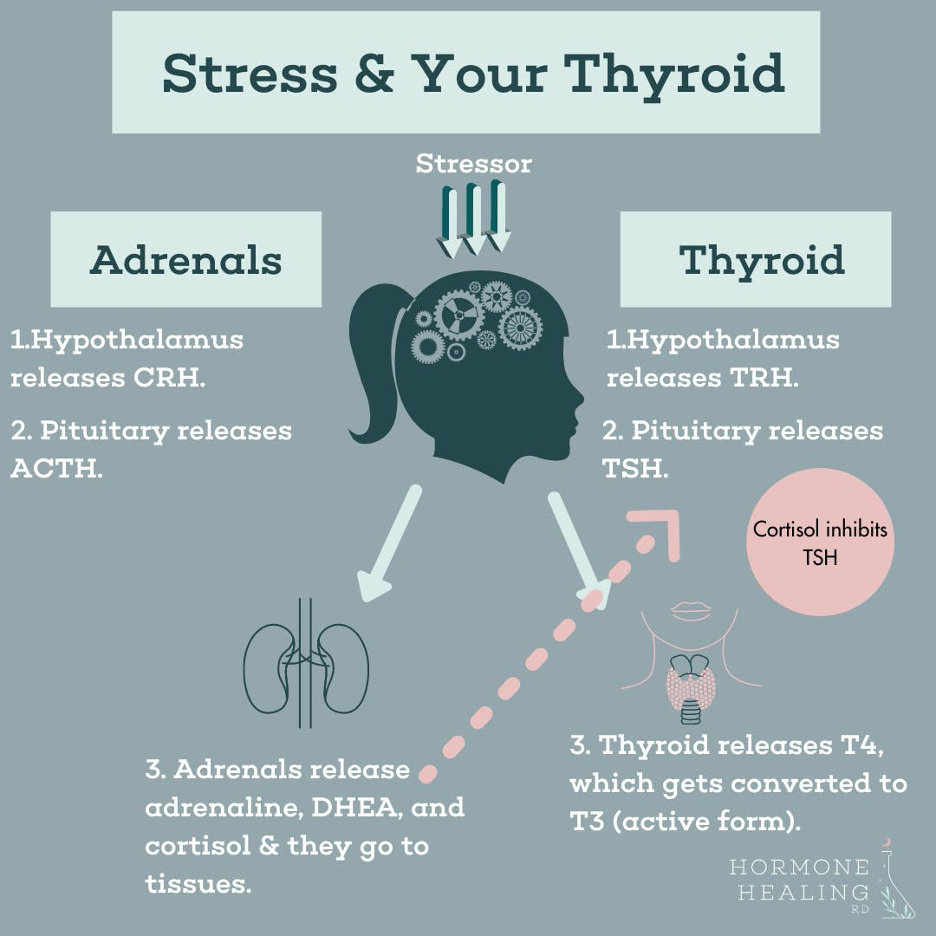
Our brain is what senses stress, then tells our hypothalamus and pituitary to talk to our adrenals and release cortisol (our stress hormone), adrenaline, and DHEA. The brain, hypothalamus, and pituitary also work with the thyroid to help produce adequate thyroid hormone. Too much cortisol disrupts the loop and inhibits thyroid function. Excess cortisol lowers thyroid-stimulating hormone production (TSH) and can even inhibit the conversion of the inactive form of thyroid hormone (T4) to the active form (T3) (see Part-1 for more on T3 conversion). For this reason, chronic stress can lead to an underachieving thyroid, worsening conditions like hypothyroidism and Hashimoto’s. When your body is under chronic stress, it responds by dialing down thyroid function. If you are dealing with thyroid issues or suspect them, first look for possible stressor(s).
Why does my lab work show normal thyroid function?
In reference to thyroid labs specifically, when we have high levels of cortisol, this will lower circulating thyroid-stimulating hormone (TSH) levels. Typically, TSH is a marker the doctor tests for when you suspect thyroid issues. It is released by our pituitary gland when our brain senses that we don’t have enough thyroid hormone in the body. When TSH goes up, it means we need more thyroid hormone. The issue is that we can be under-producing thyroid hormone, but have our TSH looks normal because we are also making a lot of cortisol. Remember, cortisol lowers TSH. Eventually, chronic high cortisol can lead to high TSH. Still, I see women with pretty severe symptoms like hair loss, irregular cycles, heavy/painful periods, constipation, low appetite, and overall just not feeling well, and they have “normal” TSH levels.

Taking this one step further, when we have chronic stress that leads to high cortisol over a long period, this increases inflammatory markers and calcium, binding to thyroid receptors. This means the thyroid hormone you’re making cannot bind, but will not show up on a normal thyroid test. One marker you can look at is reverse T3. This will increase over time with chronic stress. One way I see this in clients is with high calcium on a hair mineral test, which means calcium is leaving the bones and teeth (commonly seen with chronic stress and/or inadequate calcium intake in the diet).
I am sure you have heard the expression, “always trust your gut.” The same applies to your thyroid health. All of this is to say that if your thyroid labs are within the normal range, but your gut tells you there is something deeper going on, listen to your gut. What would the next steps be if you want to work on this? Here’s what I recommend:
It is not unusual to experience apparent symptoms of thyroid dysfunction but have your lab work to come back, indicating everything is normal. I see it all the time. The cause of these symptoms is that your body is compensating for added stress hormone levels, particularly cortisol. To get to the bottom of the compensation, I recommend assessing your nutrition and stress and getting a functional test (hair mineral analysis).
3 Ways to Work With Us
Mineral Healing Journey: A 6-Month, High-Touch Program for Women Ready to Rebalance Their Hormones at the Root
If you’re dealing with irregular cycles, PCOS, stubborn weight gain, low energy, thyroid issues, or hormone chaos, and you’re still in your cycling years, this is our most comprehensive hormone recalibration program. We’ll coach you through strategic nourishment, mineral repletion, and strength training to rebuild your metabolism and restore balance.
[Learn More About Mineral Healing Journey]
Nurture Your Fertility
Our 12-Month Advanced Fertility Program for Women Who’ve Tried Everything
If you’ve been trying to conceive for years, have experienced loss, failed cycles, or unexplained infertility, or feel like you’re “doing everything right” but still not getting pregnant, this is for you.
We focus on metabolic repair, mineral balance, inflammation, detoxification, and cellular healing, all tailored to your labs and history for BOTH partners.
[Learn More About Nurture Your Fertility]
Master Your Minerals
Self-Paced Education for Women Who Want to Understand Their Body
If you’re not ready for our group coaching but know your symptoms aren’t random, this is where to start. Master Your Minerals is our comprehensive, self-paced course that teaches you how minerals impact your hormones, metabolism, energy, and fertility.
You’ll get symptom trackers, practical tools, and structured guidance so you can start connecting the dots on your own. This is best for women who are proactive, want education first, and prefer to implement at their own pace.
